|
Additional therapies that have shown beneficial effect with low-quality evidence include iontophoresis, phonophoresis, ice massage, ultrasound therapy, periosteal pecking, and extracorporeal shockwave therapy. There are no specific recommendations on the duration of rest required for resolution of symptoms, and it is likely variable depending on the individual. 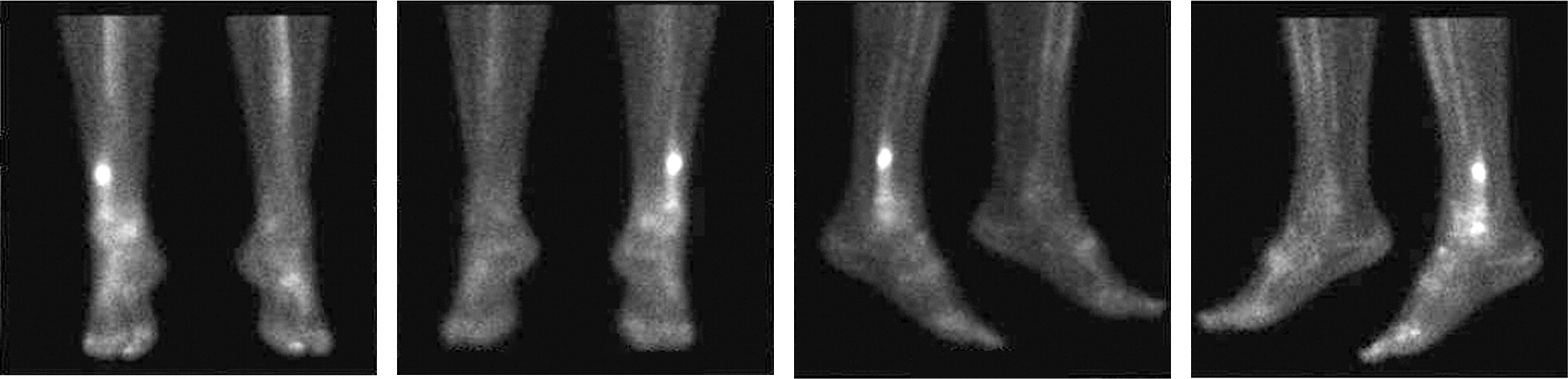
Management of medial tibial stress syndrome is conservative, mainly focusing on rest and activity modification with less repetitive, load-bearing exercise. Evaluating for vitamin D deficiency may also be warranted, especially for recalcitrant cases. High-resolution CT is another viable advanced imaging option, but with lower sensitivity than MRI or nuclear bone scan. Nuclear bone scans demonstrate increased radionuclide uptake in the cortical bone with characteristic “double stripe” pattern. MRI findings include periosteal edema and bone marrow edema. Nuclear bone scans are a reasonable alternative but are less specific and sensitive than MRI. MRI is the preferred imaging modality for identifying MTSS as well as a higher grade bone stress injury such as a tibial stress fracture. Radiograph findings of the "dreaded black line" is indicative of stress fracture. Plain radiographs are normal in patients with MTSS and are often normal with an early stress fracture. 
In particular, the situation warrants imaging if concerned for a more significant tibial stress injury. However, imaging is often performed if uncertain of etiology or to rule out other common exercise-induced lower extremity injuries. Medial tibial stress syndrome is a clinical diagnosis and can be reliably made by history and physical examination findings.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
